After having one or more permanent teeth extracted, there is a chance that you could develop a condition known as a dry socket, or alveolar osteitis. Luckily this condition is both temporary and treatable, and it should not cause any permanent damage. Nevertheless, it is important to familiarize yourself with dry sockets, especially if you are going to or have had a tooth extraction. Here is everything you need to know about a dry socket:
What is a dry socket?
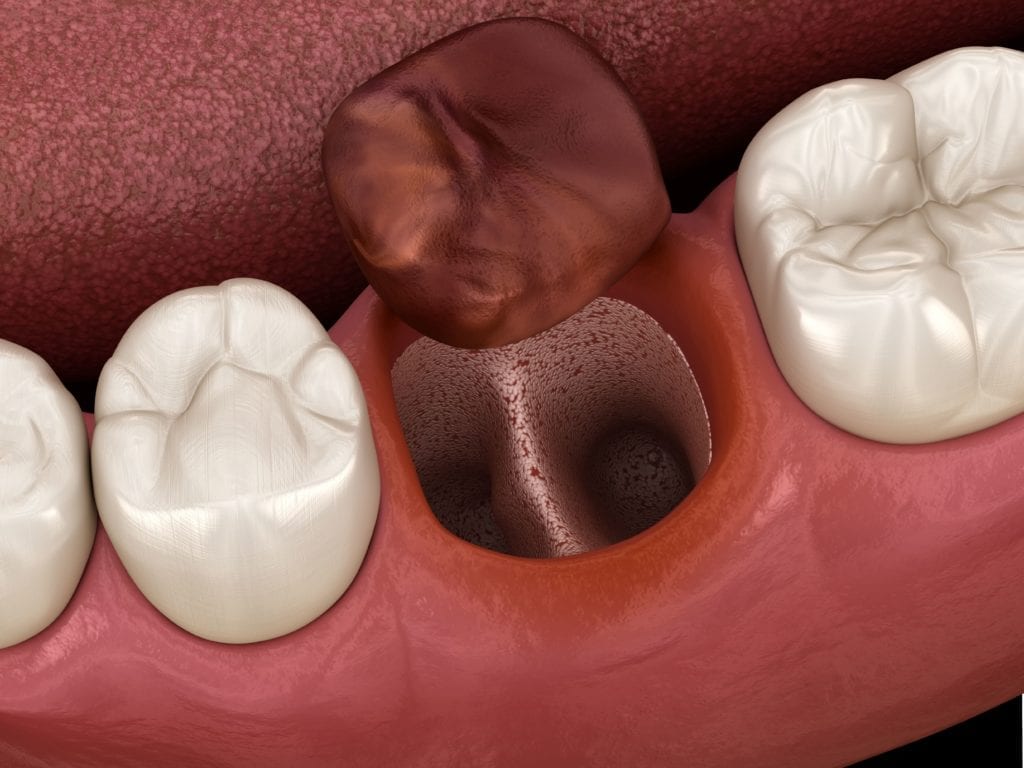
After you have a tooth extracted, the body forms a blood clot in the empty socket in order to protect the underlying bone and nerves. A dry socket occurs when this blood clot either fails to form or is dislodged and the bone and nerves are exposed.
Do I have a dry socket?
If you can look in the mirror and see bone where your tooth used to be, then you likely have a dry socket. Additionally, if you are experiencing a deep, throbbing pain in your jaw or in your ears, eyes, neck, or temple on the same side as the extraction, this can also indicate the presence of a dry socket. Bad breath or a foul taste in the mouth is another key indicator of a dry socket.
How is a dry socket treated?

If you suspect you may have a dry socket, you will need to notify your dentist as soon as possible. Your dentist will then examine the socket to determine if the blood clot has dislodged and to check for signs of infection. They will then proceed to clean the socket before packing it with gauze and medication. Packing the socket will help to alleviate pain and prevent infection. Your dentist will likely also provide you with information on how to clean the socket with salt water rinses, as well as how to pack the socket on your own.
Although most dry sockets are not serious, there are some cases where they can cause complications such as delayed healing or an infection that starts in the socket and spreads to the bone. For this reason, it is important to seek treatment for a dry socket.
How can I prevent a dry socket?
The exact cause of dry sockets is still being researched, however there are some factors that have been found to increase the risk of developing a dry socket. These include:
- Excess bacteria around the extraction site
- Trauma either during or after the extraction
- Using tobacco products, which delay healing
- Using oral contraceptives, which contain high levels of estrogen that disrupts healing
- Having a past history of dry sockets
To decrease your risk of developing a dry socket, your dentist will provide you with postoperative instructions to follow after your extraction. These instructions provide guidance on what to eat and drink after an extraction, how to manage postoperative pain, and how to keep the extraction site clean. They also contain information on the types of activities that should be avoided to prevent a dry socket such as rigorous activity, drinking from a straw, and smoking. Although following these instructions will not guarantee the absence of a dry socket, it can significantly reduce the risk.

Dr. Admar holds dual certificates — a Bachelor of Dental Surgery (BDS) in 2010 from India and a Doctor of Dental Surgery (DDS) in 2014 from Canada. He is now a full time practicing dentist in Kamloops where he provides a variety of services. Dr. Admar spends hundreds of hours in continued dental education to stay up to date in cosmetic and implant dentistry and he has achieved several advanced qualifications.


